July 2017

Population health is commonly defined as “the health outcomes of a group of individuals, including the distribution of such outcomes within the group” (Kindig and Stoddart 2003). This general definition is widely accepted and has been formally adopted by the National Academies’ Roundtable on Population Health Improvement. However, in practice, different stakeholders use the term ‘population health’ in markedly different ways. These differences are largely driven by which group of individuals is identified as the population of interest and which interventions are being pursued to influence the health outcomes of that population.
Same Words, Different Meanings
Health care insurers and providers often use the term population health to describe efforts to improve the effectiveness and accountability of the health care services they finance or deliver. In this usage, the population referenced is the group of people enrolled in a particular health plan, or the patients served by a particular provider or health system. Health care insurers and providers typically seek to influence population health outcomes through improvements in the delivery of health care services, such as accelerating the adoption of evidence-based practices, implementing chronic disease management programs, and coordinating care more effectively among service providers and modalities (Sharfstein 2014; Stoto 2013). These efforts to improve population health sometimes include new types of preventive or supportive services designed to augment the medical care for which insurers and providers have traditionally been responsible. Yet, for the most part, such services remain limited to interventions delivered to individuals within clinical settings and typically do not address the social and physical environments in which people live, learn, work, and play.
To governmental public health agencies at the local, state, and federal levels, population health is based on a geographically defined population residing within a particular jurisdiction. In addition to providing health care services to the poor and underserved, these public health agencies have historically focused on monitoring population health outcomes and addressing certain communal risks that threaten population health, by ensuring clean water, regulating food safety, and reducing the spread of infectious diseases. Some public health officials use the terms population health and public health interchangeably, but others feel that ‘public health’ is too closely associated with the direct responsibilities of governmental public health agencies. While public health agencies maintain a preventive orientation, they typically do not have the authority or resources to address the full range of socioeconomic and environmental factors that determine a population’s health status, such as income, education, housing, access to healthy foods, recreational facilities, and social supports.
Health funders have come to employ an inclusive, holistic vision for population health. This vision incorporates and expands on the traditional roles of both the health care delivery system and governmental public health agencies—and also encourages broader private- and public-sector collaboration. This perspective recognizes that responsibility for population health is shared across many sectors, and, therefore, accountability for health outcomes must be diffused (Stoto 2013). Growing attention to disparities in “the distribution of outcomes within the group” has led many health funders to focus their population health investments on health equity goals.
A Picture Is Worth a Thousand Words
A variety of frameworks and models have been developed to conceptualize this broad, cross-sectoral vision for population health, such as the Institute for Healthcare Improvement’s Model of Population Health, shown in Figure 1 (Stiefel and Nolan 2012).
Figure 1: Model of Population Health
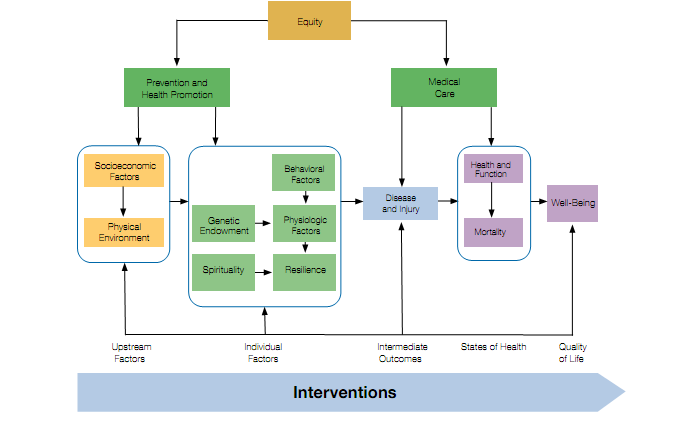
Source: Stiefel M, Nolan K. A Guide to Measuring the Triple Aim: Population Health, Experience of Care, and Per Capita Cost. IHI Innovation Series white paper. Cambridge, Massachusetts: Institute for Healthcare Improvement; 2012.
This model provides a useful overview of the determinants and intervention opportunities that shape population health, but it is not drawn to scale. Medical care contributes less than 20 percent to total influences on health outcomes, yet more than 90 percent of health expenditures are devoted to medical services (McGovern, Miller, and Hughes-Cromwick 2014). Conversely, nonclinical factors, such as socioeconomic conditions, physical environments, and behaviors, account for an estimated 80 percent of total influences on health outcomes, and receive less than 10 percent of total health funding.
Moving Upstream Together
In the past, health foundations’ funding priorities mirrored those of the overall health system, but health funders are increasingly focusing their investments on the upstream determinants of health (i.e., the socioeconomic and environmental factors that influence health outcomes). Seeking to embed and elevate health considerations within the policies and practices of other sectors, these efforts rely on cross-sector collaboration. For many funders, this work emphasizes helping health system stakeholders (public health agencies, health care providers, and health insurers) contribute their expertise and financial resources to multi-sector partnerships that adopt a broad vision of population health.
For example, in 2015 the Robert Wood Johnson Foundation (RWJF), the Kresge Foundation, the de Beaumont Foundation, the Colorado Health Foundation, and the Advisory Board launched the BUILD Health Challenge, bringing community-based nonprofits together with both their local public health departments and their hospitals to identify bold, upstream, innovative, local, data-driven solutions to health problems. A key feature of BUILD funding requires partnering hospital systems to provide a 1:1 match in support for each award. BUILD has funded implementation projects in 17 cities to address a range of issues, such as housing improvement, transportation, and violence prevention. A second round of funding is underway in 2017 with support from seven additional funders (Slonim 2017).
In a similar effort, a consortium of California funders, The California Endowment, Blue Shield Foundation of California, and Kaiser Permanente, is jointly funding the California Accountable Communities for Health Initiative (CACHI), which seeks to link clinical services, community programs, and social services with public health and primary prevention approaches to collectively address a particular health need on a communitywide basis. In 2016, six local communities from across the state were awarded up to $850,000 each over three years to advance common health goals and create a vision for a more expansive, connected, prevention-oriented health system. Community-defined priorities include asthma, violence, obesity and cardiovascular disease.
These types of multisector partnerships appear to be proliferating across the country. ReThink Health, an initiative of the Rippel Foundation, recently published their 2016 Pulse Check on Multi-Sector Partnerships, which found rapid growth of these efforts (Erickson et al. 2017). Of the more than 200 partnerships surveyed, most (65 percent) have formed within the last six years. Nearly a third of these partnerships (29 percent) are comprehensive in nature, meaning they address health care, health behaviors, socioeconomic conditions, and physical environments. An additional 36 percent include a mix of activities targeting two to three of these areas.
A variety of resources are available to support multisectoral partnerships. For instance, ReThink Health has developed multiple tools to facilitate partnership development and implementation, such as a financing primer that explores strategies for securing sustainable funding and a Dynamics Model that simulates the potential impact of different intervention and investment options. The Practical Playbook, developed by the Duke University School of Medicine and supported by the de Beaumont Foundation, advances collaboration among public health, primary care, and others to improve population health by offering strategic guidance, training resources, useful tools, national convenings, and success stories to encourage and accelerate collaborative efforts.
In order to achieve meaningful, sustainable improvements in population health, health funders are increasingly venturing out of their comfort zone to engage in new issues and cultivate new partnerships. This realignment has been challenging for many, requiring health funders to gain expertise in previously unfamiliar areas and to develop relationships with previously unknown partners. Some foundations are just beginning to grapple with their role in supporting upstream interventions. Although the complexity of population health determinants may seem daunting, many paths lead upstream. Funders can learn from their peers, and from a growing evidence base, to identify the priorities and strategies that are most likely to improve population health in the communities they serve.
References
Erickson, Jane, Bobby Milstein, Lisa Schafer, Katy Evans Pritchard, Carly Levitz, Creagh Miller, and Allen Cheadle. 2017. Progress Along the Pathway for Transforming Regional Health: A Pulse Check on Multi-Sector Partnerships. ReThink Health.
Kindig, D., and G. Stoddart. 2003. What is population health? Am J Public Health 93 (3):380-3.
McGovern, Laura, George Miller, and Paul Hughes-Cromwick. 2014. Health Policy Brief: The Relative Contribution of Multiple Determinants to Health Outcomes. Health Affairs.
Sharfstein, J. M. 2014. The strange journey of population health. Milbank Q 92 (4):640-3.
Slonim, Amy. 2017. Aligning Philanthropy To Support Locally Driven Health Interventions Addressing Upstream Issues. In Grant Watch: Health Affairs.
Stiefel, Matthew, and Kevin Nolan. 2012. A Guide to Measuring the Triple Aim: Population Health, Experience of Care, and Per Capita Cost. IHI Innovation Series white paper.
Stoto, Michael A. 2013. Population Health in the Affordable Care Act Era.
Focus Areas:
Topics:

