Upcoming Events
Past Events
Latest Resources
A Philanthropic Tree of Life: Seeding Health Equity through Influence and Innovation
Philanthropy can function as a living ecosystem for change rooted in equity, nourished by trust, and bearing the fruits of community well-being. The Direct Relief Fund for Health Equity (DRFHE), launched with $50 million in initial investments, exemplifies a transformative philanthropic model supporting nearly 200 community-based organizations across the United States. Acknowledging DRFHE as a “Tree of Life” offers a framework grounded in community-led, trust-based, and unrestricted giving that challenges traditional philanthropic paradigms. Therefore, this article describes the fund’s origins, strategic priorities, and outcomes, and introduces the DRFHE Tree of Life framework as a replicable model for equity-driven philanthropy.
Pottstown Regional Community Foundation: August 2025
The Pottstown Regional Community Foundation (PRCF) will launch its 2025 Fall Grant Round. For this final grant round of the calendar year, the foundation prioritizes organizations that demonstrate clear alignment with PRCF’s Results Framework and have not yet received an award this calendar year. Competitive requests will be supported by goals stated in community and regional plans and address needs communicated in foundation or other research studies.
Cara V. James Speaks Up on Federal Disruption with Inside Philanthropy
Grantmakers In Health (GIH) President and CEO Cara V. James was interviewed for an Inside Philanthropy article published on April 30, 2025. The piece outlines philanthropy’s reactions to the sweeping cuts to public health infrastructure in the United States, the consequences of these cuts, and the importance of remaining committed to our values.
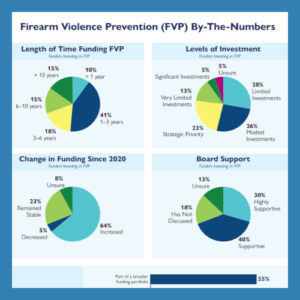
New Grantmakers In Health Survey Finds a Significant Growth in Firearm Violence Prevention Investments Among Health Funders
Washington, DC, March 14, 2025—At a time when firearm violence is a leading cause of death for children and teens, a new Grantmakers In Health survey of health funding organizations found that philanthropic investments in firearm violence prevention are growing in terms of both the number of funders supporting this work and the dollar amounts…
Let’s Take Courageous Steps Together in 2025
At the Kate B. Reynolds Charitable Trust, this has been a challenging year for North Carolina, where we live and work. Hurricane Helene devastated the western part of NC and the surrounding region, and we endured an election that divided our state and nation.
We also know that we are not alone facing the challenges of 2024 and those we will take on in 2025. Many of us in the Grantmakers In Health (GIH) community are wondering how to persevere through these uncertain times. At the Trust, we acknowledge the heaviness of the moment—because we anticipate policy changes that will negatively impact people who are already being left behind.
Postpartum Care Systems: Strategically Collaborating to Advance and Align Solutions Across Sectors
As state policymakers began extending continuous eligibility for postpartum Medicaid coverage from the 60 days following birth to the 12 months following birth in 2022, a small workgroup of
funders connected to explore what philanthropy’s role could be in strengthening maternal health outcomes
and how we might support effective implementation of the extension
Q&A: How the Chicago South Side Birth Center is Championing a Better Approach to Maternal Health
Grantmakers In Health (GIH) recently spoke with Jeanine Valrie Logan, Founder + Lead Steward of the Chicago South Side Birth Center, and Shruti Jayaraman, Chief Investments Officer of Chicago Beyond, to learn how the Chicago South Side Birth Center and Chicago Beyond are working together to improve maternal health outcomes for mothers in one of Chicago’s most underserved communities. This interview has been edited for style and clarity.
Illinois Children’s Healthcare Foundation’s Persistent Journey toward Equity
Since 2019, the Illinois Children’s Healthcare Foundation (ILCHF) has embarked upon a journey of perspective transformation—challenging ourselves to know, think, and believe differently so we will decide, engage, and act more equitably. Through consistent commitment and action, our Board of Directors, leadership, and staff have moved equity, diversity, and inclusion (EDI) work beyond “box checking” activities, institutionalizing long-term, individual, organizational, community, and cultural changes.
New Grantmakers In Health Survey Finds Leadership and Staff of Health Funders More Diverse than Broader Philanthropic Field
A new Grantmakers In Health survey of health funder leadership, staff, and boards found that health funder organizations are more racially and ethnically diverse than the broader field of philanthropy.
Connect With Funder Peers on Health Equity
Interested in exchanging strategies, information, and questions with your funder peers? Sign up for GIH E-Forums.
Strengthen your knowledge, skills, and capacity.
GIH focuses our programming around five areas that are critical to achieving better health for all.
We invite you to explore the resources available on our focus areas pages, browse content in more specific issue areas, and to connect with GIH staff to discuss how we can partner and support your work.