Latest Resources
The Commonwealth Fund: August 2024
The 2024 State Scorecard on Women’s Reproductive Health has been released based on the most recent data to assess how well the health care system is working for women in every U.S. state. It measures performance by 32 different metrics across three areas: health outcomes; health care quality and prevention; and coverage, access, and affordability.
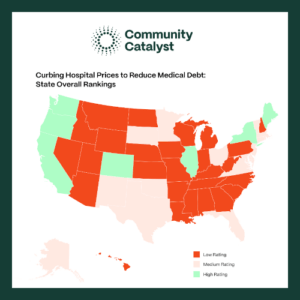
A Compendium of State Policies to Curb Hospital Prices and Reduce Medical Debt
Health care in the United States is the most expensive in the world by far and the reason is simple – health care providers keep increasing the prices of services. Hospitals, which represent the largest component of health care spending, have an outsized influence on medical debt in their communities through their policies and behavior.
As More Americans Gain Health Care Coverage, Advocates Fight for Higher-Quality Insurance
People’s Action and our allies fought hard to win health care for millions through the Affordable Care Act and Medicaid expansion. 91 percent of Americans now have health insurance, even though there is still work to do to ensure everyone can get coverage, particularly immigrants and those living in holdout non-expansion states.
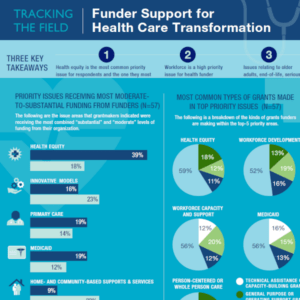
Funder Support for Health Care Transformation
This infographic summarizes the responses to a Grantmakers In Health funder poll, conducted October 2022, on how philanthropy is supporting health care transformation efforts, especially those concerned with improving quality of life, coordinating complex care, and taking patient preferences into account.
AHRQ Releases Annual Update on U.S. Healthcare Quality, Disparities
The Agency for Healthcare Research and Quality has released its National Healthcare Quality and Disparities Report, which details the state of healthcare quality and disparities in the United States. The report identifies improvements in HIV and colon cancer care, nursing home care, and medication prescribing to older adults. The report also indicates that more work needs to be done to address disparities in important areas. Among the findings, dental and oral health care services have not substantially improved, particularly for people with low income or who live in rural areas.
Reimagining A Quality Information System For US Health Care
Recommendations include: a national data infrastructure that operates independent of practice setting; aligned multipayer incentives that support needed infrastructure investments; longitudinal patient-reported outcome measures captured both in-clinic and through mobile technologies; a series of robust regional demonstration projects to broaden stakeholder understanding and technical capability; and a governance mechanism that assures both simplification and alignment of methods.
Connect With Funder Peers on Quality
Interested in exchanging strategies, information, and questions with your funder peers? Sign up for GIH E-Forums.